Understanding Urodynamic Study: A Comprehensive Guide to Bladder Function Assessment: When it comes to diagnosing and treating urinary tract problems, urodynamic studies play a crucial role in providing valuable insights into bladder function. This comprehensive guide will walk you through the fundamentals of urodynamic study, its importance, procedure, and how it aids in the diagnosis of various urological conditions.

When individuals face urinary tract issues, understanding the underlying causes and finding appropriate treatment options becomes crucial. Urodynamic studies, also known as bladder function assessments, are specialized tests used by healthcare professionals to evaluate the functioning of the bladder and associated structures. By measuring various parameters related to bladder pressure, flow, and capacity, urodynamic studies provide valuable information for diagnosing a range of urological conditions. In this comprehensive guide, we will delve into the intricacies of urodynamic studies, their significance, the procedure involved, interpretation of results, and their applications in urology.
What is Urodynamic Study?
A urodynamic study refers to a set of diagnostic procedures conducted to assess the function and performance of the urinary system. It involves measuring and evaluating various aspects such as bladder pressure, urine flow rate, bladder capacity, and the coordination between the bladder and urethral sphincters.
Importance of Urodynamic Study:
Urodynamic studies play a critical role in identifying the underlying causes of urinary tract problems and enable healthcare professionals to make accurate diagnoses. They provide valuable insights into the function of the bladder and help differentiate between different urological conditions such as urinary incontinence, bladder outlet obstruction, and neurogenic bladder dysfunction.
Bladder Function Assessment:
The test provides valuable information about bladder capacity, pressure during filling and voiding, and the coordination between the bladder and urethra. Urodynamic studies are particularly helpful in diagnosing urinary incontinence, bladder overactivity, and other bladder-related issues.
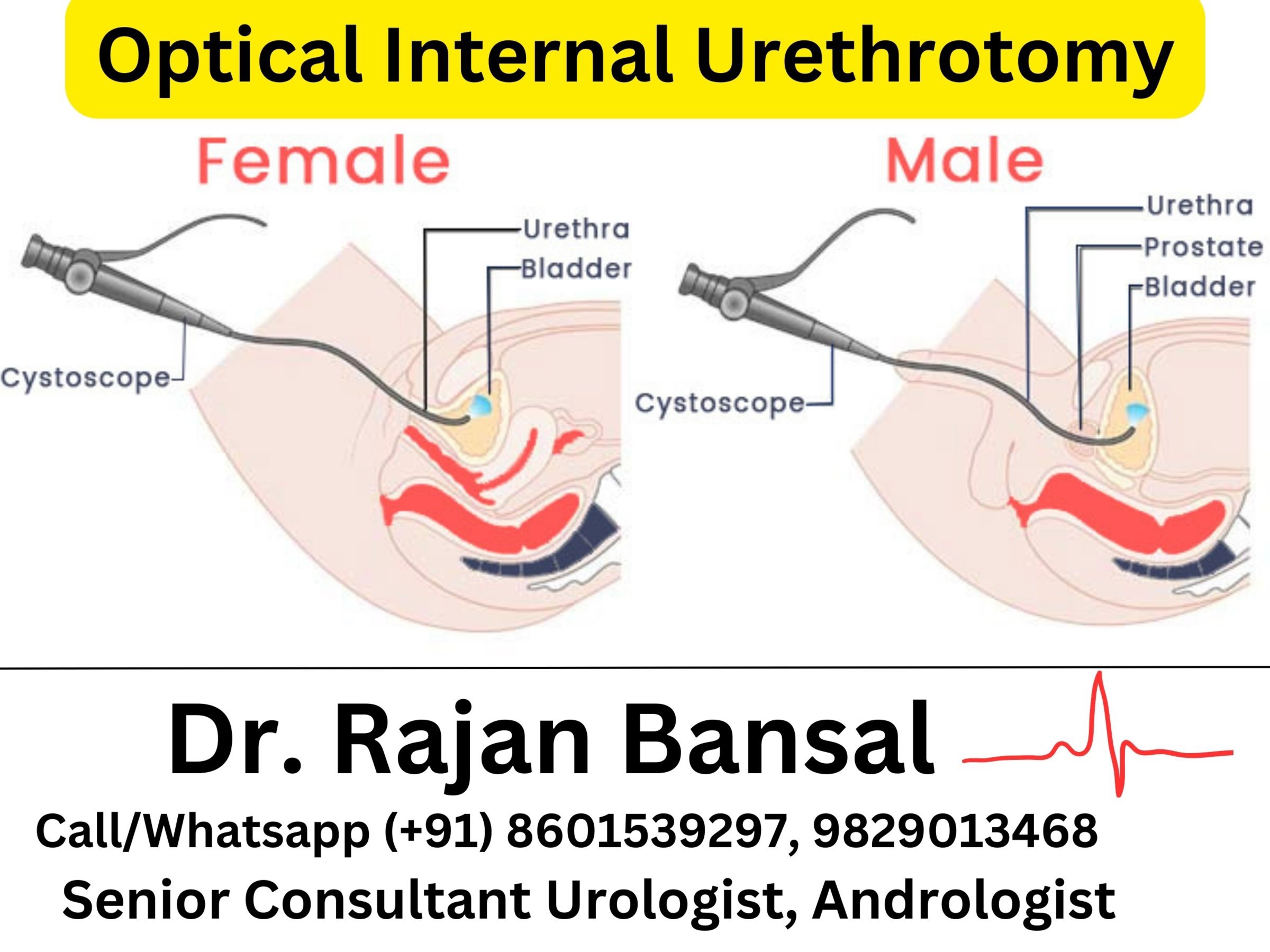
Anatomy of the Urinary Tract:
To understand urodynamic studies, it is essential to have a basic understanding of the anatomy of the urinary tract. The urinary tract consists of various components, including the kidneys, ureters, bladder, and urethra. The kidneys filter waste products and excess fluids from the bloodstream, producing urine. The urine travels through the ureters, which are thin tubes connecting the kidneys to the bladder. The bladder acts as a storage organ for urine, expanding as it fills and contracting to empty the urine through the urethra, a tube that connects the bladder to the outside of the body.
Normal Bladder Function
In a healthy individual, the bladder undergoes a coordinated cycle of filling and emptying. As the bladder gradually fills with urine, the muscles in the bladder wall stretch to accommodate the increasing volume. Once a certain threshold is reached, the individual experiences the sensation of needing to urinate. During the emptying phase, the bladder contracts while the urethral sphincter relaxes, allowing urine to flow out.
Understanding Common Urological Conditions
Urodynamic studies are particularly useful in diagnosing various urological conditions that affect bladder function. Some common conditions include:
Urinary Incontinence: This refers to the involuntary leakage of urine. Urodynamic studies can help determine the underlying cause of urinary incontinence, such as stress incontinence (leakage with physical exertion), urge incontinence (sudden and intense urge to urinate), or mixed incontinence (a combination of both).
Bladder Outlet Obstruction: This condition occurs when there is a blockage or narrowing of the urethra, impeding the flow of urine from the bladder. Urodynamic studies can assess the pressure and flow patterns to identify the presence and severity of obstruction.
Neurogenic Bladder Dysfunction: Neurological conditions such as spinal cord injury, multiple sclerosis, or stroke can disrupt the communication between the bladder and the nervous system, leading to problems with bladder control. Urodynamic studies can evaluate the coordination between the bladder muscles and the sphincters, helping to guide treatment options.
The Urodynamic Study Procedure
- Preparing for the Study
- Filling Phase
- Storage Phase
- Voiding Phase
- Pressure-Flow Study
- Post-void Residual Measurement
- Additional Urodynamic Tests
A urodynamic study typically involves several phases to assess different aspects of bladder function. While specific procedures may vary, the general steps involved are as follows:
Preparing for the Study:
Before undergoing a urodynamic study, your healthcare provider will provide instructions on necessary preparations, such as emptying your bladder before the procedure and avoiding caffeine or certain medications that may affect bladder function.
Filling Phase:
During the filling phase, a small catheter is inserted into the bladder through the urethra, and another catheter may be placed in the rectum or vagina to measure abdominal pressure. The bladder is then slowly filled with sterile fluid while various measurements are recorded, such as bladder volume, pressure, and sensations.
Storage Phase:
Once the bladder is adequately filled, the storage phase begins. During this phase, the healthcare provider observes and measures the bladder’s ability to hold urine without leakage. The patient may be asked to perform certain activities, such as coughing or changing positions, to assess bladder control.
Voiding Phase:
After the storage phase, the patient is asked to empty their bladder. The healthcare provider measures the urine flow rate, and the pressure in the bladder and urethra is recorded. This phase helps evaluate the coordination between the bladder muscles and the urethral sphincter during the emptying process.
Pressure-Flow Study:
In some cases, a pressure-flow study may be conducted to assess bladder and urethral function during urination. This involves measuring the pressure inside the bladder and the flow rate of urine simultaneously. The results help determine if there are any obstructions or abnormalities affecting the flow of urine.
Post-void Residual Measurement:
After the voiding phase, a post-void residual (PVR) measurement may be taken. This involves using an ultrasound or catheter to determine the amount of urine remaining in the bladder after emptying. A high PVR volume may indicate incomplete bladder emptying or other underlying issues.
Additional Urodynamic Tests:
Depending on the specific needs of the patient, additional urodynamic tests may be performed. These may include electromyography (EMG) to measure muscle activity in the pelvic floor or sphincters, cystometrogram (CMG) to assess bladder pressure and capacity, or leak point pressure measurement to evaluate urinary leakage under stress or increased abdominal pressure.
Interpreting Urodynamic Study Results
After the urodynamic study, the recorded data is analyzed by our expert urologist. Several parameters are assessed, including bladder capacity, compliance, detrusor pressure, urine flow rate, and urethral function. The results are interpreted to identify any abnormalities or dysfunctions in bladder control, urinary flow, or sphincter function.
Urodynamic Parameters:
Bladder Capacity: The maximum volume the bladder can hold before the sensation of needing to urinate.
Detrusor Pressure: The pressure generated by the bladder muscles during filling and emptying.
Compliance: The ability of the bladder to expand and contract without significant increases in pressure.
Urine Flow Rate: The speed at which urine flows out during voiding.
Urethral Pressure: The pressure exerted by the urethra to maintain continence.
Detrusor Overactivity:
Detrusor overactivity refers to the involuntary contraction of the bladder muscle during the filling phase, leading to urgency, frequency, and potential urinary leakage. Urodynamic studies can help diagnose and assess the severity of detrusor overactivity, aiding in the development of appropriate treatment strategies.
Bladder Outlet Obstruction:
Urodynamic studies are particularly effective in detecting bladder outlet obstruction, which occurs when there is an obstruction or narrowing of the urethra that hinders urine flow. Elevated detrusor pressure, decreased urine flow rate, and difficulty emptying the bladder are indicative of this condition.
Stress Urinary Incontinence:
Stress urinary incontinence refers to the leakage of urine during activities that increase abdominal pressure, such as coughing, sneezing, or physical exertion. Urodynamic studies can help determine the underlying cause of stress urinary incontinence, such as weakened pelvic floor muscles or inadequate urethral closure.
Neurogenic Bladder Dysfunction:
Urodynamic studies are invaluable in assessing neurogenic bladder dysfunction, which occurs due to neurological conditions that disrupt the communication between the bladder and the nervous system. Abnormal patterns of detrusor contractions, sphincter function, and coordination between the bladder and sphincters can help identify the specific type and severity of neurogenic bladder dysfunction.
Applications of Urodynamic Study
Urodynamic studies have several significant applications in the field of urology:
Diagnosis of Bladder Dysfunction:
Urodynamic studies aid in the diagnosis of various bladder dysfunctions, including urinary incontinence, bladder outlet obstruction, neurogenic bladder, and other complex urological conditions. Accurate diagnosis allows healthcare providers to tailor treatment plans based on the specific needs of each patient.
Treatment Planning:
By providing detailed information on bladder function and dysfunctions, urodynamic studies help healthcare providers develop appropriate treatment strategies. The results assist in determining whether conservative measures, medications, behavioral therapies, or surgical interventions are necessary.
Evaluating Treatment Outcomes:
Urodynamic studies can also be used to evaluate the effectiveness of treatment interventions. By repeating the urodynamic study after a certain period of treatment, healthcare providers can assess whether the chosen treatment approach has resulted in improvements in bladder function and symptoms. This information helps guide further treatment decisions and adjustments if needed.
Research and Advancements in Urology:
Urodynamic studies play a vital role in advancing the field of urology. Researchers and healthcare professionals utilize the data obtained from urodynamic studies to gain a deeper understanding of bladder function, develop new diagnostic techniques, refine treatment approaches, and explore innovative interventions for various urological conditions.
Risks and Considerations
Potential Risks and Discomfort:
Urodynamic studies are generally considered safe, but as with any medical procedure, there are potential risks and discomforts involved. These may include urinary tract infection, temporary bladder discomfort or urgency, and rare complications such as bladder perforation. However, these risks are minimal and healthcare providers take precautions to minimize discomfort and ensure patient safety.
Contraindications for Urodynamic Study:
While urodynamic studies are generally safe, there are certain situations where they may not be recommended. These include active urinary tract infection, severe bleeding disorders, or recent pelvic surgery. Your healthcare provider will assess your individual situation and determine if a urodynamic study is appropriate for you.
Alternative Diagnostic Methods:
In some cases, alternative diagnostic methods may be considered, depending on the specific symptoms and clinical presentation. These may include imaging studies such as ultrasound or cystoscopy, which can provide additional information about the urinary system.
Preparing for a Urodynamic Study
Communicating with Your Urologist:
Before undergoing a urodynamic study, it is essential to communicate openly with your urologist. Discuss any symptoms, concerns, or medical conditions you may have. This information will help them tailor the urodynamic study to your specific needs.
Understanding the Procedure:
Ask your urologist to explain the urodynamic study procedure in detail. Understanding what to expect during the study, including the use of catheters and the sensations you may experience, can help alleviate anxiety and ensure a more comfortable experience.
Addressing Concerns and Questions:
If you have any concerns or questions about the urodynamic study, do not hesitate to discuss them with your doctor. They can provide further information, clarify any doubts, and help you feel more confident and informed about the procedure.
Advanced Urodynamic Study Laboratory in Jaipur – Institute of Urology, C Scheme, Jaipur
Urodynamic studies are invaluable diagnostic tools that provide critical insights into bladder function and aid in the diagnosis and management of various urological conditions. By assessing bladder pressure, flow, and coordination, these studies assist urologists in developing tailored treatment plans and monitoring treatment outcomes. While the procedure may involve some discomfort, the benefits of urodynamic studies far outweigh the minimal risks. If you are experiencing urinary tract problems, consult your urologist to determine if a urodynamic study is right for you.
If you are experiencing urinary tract problems, do not hesitate to contact me at 8601539297 (Dr. Rajan Bansal) and discuss the potential benefits of a urodynamic study. Understanding your bladder function through urodynamic studies can lead to accurate diagnoses, personalized treatment plans, and improved quality of life. You can also come and consult with me at Institute of Urology, Jaipur. Personalised appointments can be booked at 9829013468.
Remember, taking proactive steps towards understanding and managing your bladder health is key to maintaining overall well-being.