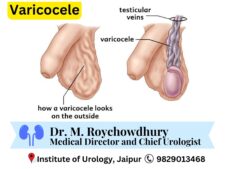
Testicular Tumors: Exploring Types, Causes, and Diagnosis for Early Intervention: Testicular tumors, though relatively rare, can have a significant impact on a man’s health and well-being. Understanding the different types, causes, and effective diagnostic approaches is crucial for early detection and appropriate treatment. This comprehensive article delves into the world of testicular tumors, shedding light on the various types, exploring their underlying causes, and highlighting essential diagnostic methods to ensure timely intervention and improved outcome

What are Testicular Tumors?
Testicular tumors are abnormal growths that develop in the testicles, which are the male reproductive organs responsible for producing sperm and testosterone. Testicular tumors can be benign (non-cancerous) or malignant (cancerous). The majority of testicular tumors are malignant, with testicular cancer being the most common type of cancer in young and middle-aged men.
Types of Testicular Tumors
Testicular tumors can be classified into different types based on the specific cells or tissues from which they originate. The two main categories of testicular tumors are germ cell tumors and non-germ cell tumors.
A. Germ Cell Tumors:
Germ cell tumors are the most common type of testicular tumors, accounting for about 95% of cases. They develop from the cells that produce sperm. Germ cell tumors can be further divided into two subtypes:
1.Seminomas: Seminomas are slow-growing tumors that typically occur in men between the ages of 30 and 40. They tend to be confined to the testicle initially and have a high cure rate. There are two main types of seminomas:
a. Classic Seminoma: These tumors have a characteristic appearance under the microscope and respond well to treatment.
b. Spermatocytic Seminoma: This is a rare form of seminoma that tends to affect older men. It usually grows more slowly and has a good prognosis.
2. Non-Seminomas: Non-seminomatous germ cell tumors (NSGCTs) are a group of more aggressive tumors that often contain a mixture of different cell types. NSGCTs tend to occur in younger men, typically in their late teens or early twenties. The subtypes of non-seminomas include:
a. Embryonal Carcinoma: This aggressive type of tumor grows rapidly and can spread outside the testicle.
b. Yolk Sac Tumor: This type is more common in young children and has a good prognosis when diagnosed early.
c. Choriocarcinoma: This is a rare and highly malignant tumor that can spread rapidly to other parts of the body.
d. Teratoma: Teratomas are tumors that can contain different types of tissues, such as hair, muscle, or bone. They are often present in combination with other germ cell tumors.
B. Non-Germ Cell Tumors:
Non-germ cell tumors of the testicle are less common than germ cell tumors. They originate from other types of cells within the testicle. Some examples include:
1.Leydig Cell Tumors: These tumors develop from the Leydig cells, which produce testosterone. Most Leydig cell tumors are benign, but a small percentage can be malignant.
2. Sertoli Cell Tumors: These tumors arise from the Sertoli cells, which support sperm production. They are usually benign and rarely spread to other parts of the body.
3. Gonadoblastoma: This is a rare tumor that typically occurs in individuals with disorders of sex development. It contains both germ cells and sex cord-stromal cells.
It’s worth noting that the treatment and prognosis of testicular tumors vary depending on the specific type, stage, and other factors. Therefore, a proper diagnosis by a healthcare professional is crucial to determine the most appropriate treatment approach.
Causes and Risk Factors of Testicular Tumours
The exact causes of testicular tumors are not fully understood. However, several risk factors have been identified that may increase the likelihood of developing testicular tumors. These include:
Undescended Testicle (Cryptorchidism): When one or both testicles fail to descend into the scrotum before birth, it is known as cryptorchidism. Men with a history of cryptorchidism have a higher risk of developing testicular tumors compared to those with normal testicular descent. The risk is highest when both testicles are affected.
Personal or Family History: Having a personal history of testicular cancer increases the risk of developing a tumor in the remaining testicle. Additionally, having a close relative, such as a father or brother, with testicular cancer also increases the risk.
Age: Testicular tumors, particularly germ cell tumors, are more common in young and middle-aged men, typically between the ages of 15 and 40. The risk decreases with age, with older men having a lower risk.
Abnormal Testicular Development: Certain conditions that affect testicular development or hormonal balance may increase the risk of testicular tumors. These include:
Klinefelter syndrome: This genetic condition is characterized by the presence of an extra X chromosome in males (XXY instead of XY). Men with Klinefelter syndrome have a higher risk of developing testicular cancer.
Carcinoma in situ: This condition refers to abnormal cells that are confined to the lining of the seminiferous tubules (the tiny tubes where sperm cells develop). Carcinoma in situ is considered a precursor to testicular cancer and increases the risk of developing an invasive tumor.
Testicular dysgenesis syndrome: This syndrome encompasses various disorders related to testicular development, including cryptorchidism, hypospadias (abnormal opening of the urethra), and reduced sperm production. It is associated with an increased risk of testicular tumors.
Race and Ethnicity: Testicular tumors are more common in white men compared to men of other racial or ethnic backgrounds.
It’s important to note that while these risk factors may increase the likelihood of developing testicular tumors, the majority of men with these risk factors do not develop cancer. On the other hand, some individuals without any known risk factors may still develop testicular tumors. Regular self-examinations and routine medical check-ups are essential for early detection and prompt treatment if any abnormalities are noticed.
Signs and Symptoms of Testicular Tumours
Signs and symptoms of testicular tumors can vary, and it’s important to note that not all individuals will experience noticeable symptoms. However, when present, the following signs and symptoms may indicate the presence of a testicular tumor:
Testicular Lump or Swelling: The most common symptom of a testicular tumor is the presence of a painless lump or swelling in one or both testicles. The lump may feel firm or solid and can vary in size.
Heaviness or Discomfort: Some men may experience a feeling of heaviness or discomfort in the scrotum or testicle affected by the tumor. This sensation may not necessarily be painful but can be persistent or intermittent.
Pain or Discomfort: Testicular tumors can cause pain or discomfort in the affected testicle or scrotum. The pain can range from a dull ache to sharp or throbbing pain. However, it’s important to note that testicular pain can have various causes, and not all cases of testicular pain indicate the presence of a tumor.
Changes in Testicle Size or Shape: Testicular tumors can lead to changes in the size, shape, or consistency of the testicle. One testicle may become noticeably larger or smaller than the other, or there may be a change in the overall shape or contour of the testicle.
Feeling of Testicular Fullness: Some individuals with testicular tumors may experience a sensation of fullness or heaviness in the affected testicle.
Back Pain or Lower Abdominal Pain: In more advanced cases, testicular tumors can spread to nearby lymph nodes or other organs, causing symptoms such as lower back pain or lower abdominal pain.
It’s important to remember that these symptoms can also be caused by other conditions unrelated to testicular tumors. However, if you experience any of these symptoms or notice any changes in your testicles, it is recommended to seek medical attention (Call us on 8601539297 for expert opinion) for a proper evaluation and diagnosis. Early detection and treatment of testicular tumors offer the best chances for successful outcomes.
How is the Diagnosis of Testicular Tumour Made?
When a testicular tumor is suspected, several diagnostic approaches are used to evaluate the condition and determine the type, stage, and extent of the tumor. These diagnostic approaches include:
Physical Examination: An expert urologist will perform a physical examination, including a careful examination of the scrotum, testicles, and nearby lymph nodes. They will check for any abnormalities such as lumps, swelling, or changes in size or shape of the testicles.
Imaging Tests:
Ultrasound: Ultrasound imaging is commonly used as the initial imaging test for evaluating testicular tumors. It uses sound waves to create detailed images of the testicles and can help identify the presence, location, and characteristics of a tumor.
Computed Tomography (CT) Scan: CT scans may be performed to determine if the tumor has spread to nearby lymph nodes or other organs in the abdomen or pelvis.
Magnetic Resonance Imaging (MRI): MRI may be used to provide detailed images of the testicles and surrounding tissues, particularly for assessing the extent of the tumor and evaluating any nearby lymph node involvement.
Blood Tests:
Tumor Markers: Blood tests can measure certain tumor markers, which are substances produced by the tumor or released into the bloodstream. In the case of testicular tumors, commonly measured tumor markers include alpha-fetoprotein (AFP), beta-human chorionic gonadotropin (β-hCG), and lactate dehydrogenase (LDH). Elevated levels of these markers can provide valuable information about the type and extent of the tumor.
Testicular Biopsy: In some cases, a biopsy may be performed to obtain a small sample of tissue from the testicle for examination under a microscope. A biopsy helps confirm the diagnosis and determine the specific type of testicular tumor. However, testicular biopsies are not routinely performed as they can potentially cause the cancer cells to spread.
Surgical Exploration: In certain situations where the diagnosis is uncertain, surgical exploration of the scrotum and testicles may be performed to directly visualize and examine the testicular tissue. This approach allows for a more accurate diagnosis and staging of the tumor.
It’s important to note that the specific diagnostic approaches used may vary depending on the individual case and the suspected type and stage of the tumor. The results of these diagnostic tests help guide the treatment plan and determine the appropriate course of action for managing the testicular tumor.
Diagnosis and Treatment of Testicular Cancer in Jaipur – Institute of Urology, C Scheme, Jaipur
Testicular tumors demand our attention due to their potential impact on men’s health and quality of life. By understanding the various types, underlying causes, and adopting timely diagnostic approaches, we can ensure early detection and appropriate treatment, leading to improved prognosis and survival rates. Regular self-examinations, seeking medical advice for any concerning symptoms, and following up with your urologist are essential for safeguarding one’s well-being. Remember, early intervention is key to overcoming testicular tumors and maintaining a healthy, fulfilling life.
At Institute of Urology, Jaipur we are well equipped with latest technology and advance equipments to precisely confirm the diagnosis of testicular tumours. We have made it possible for patients to receive all facilities including blood investigations and imaging studies inside the hospital premises itself so that patients do not have to go place to place for different tests. Therefore, we provide Total Urology Care Under One Roof. For any questions or queries, I can be reached at 9929513468 (Dr. M. Roychowdhury). You can also come and personally consult me at the hospital. I encourage you to please take an appointment by calling at 9829013468 which would help me attend to you on a priority basis without any waiting time.