The sensation of urgently needing to urinate, often accompanied by frequent urination and sometimes even urinary incontinence, can significantly impact an individual’s quality of life. These symptoms characterize a condition known as overactive bladder (OAB), a prevalent urological issue affecting millions worldwide. This comprehensive guide aims to unravel the complexities of OAB, shedding light on its symptoms, underlying causes, available treatments, and practical management strategies.

Symptoms of Overactive Bladder:
Individuals experiencing OAB often encounter bothersome symptoms, such as
- a sudden and urgent need to urinate (urgency),
- frequent urination (frequency),
- and sometimes involuntary leakage of urine (urge incontinence).
These symptoms can disrupt daily routines, leading to emotional distress and affecting one’s social life and self-confidence.
Causes and Risk Factors:
The exact cause of OAB remains multifactorial, involving a combination of physiological, neurological, and lifestyle factors. Conditions such as bladder infections, neurological disorders (like Parkinson’s disease or stroke), pelvic floor dysfunction, and even certain medications or dietary habits may contribute to the development or exacerbation of OAB. Age, gender, and individual lifestyle choices also influence the risk of developing this condition.
- Muscle and Nerve Issues: Dysfunction in the muscles of the bladder or abnormalities in nerve signals between the brain and the bladder can lead to OAB. This includes involuntary contractions of the bladder muscles, causing a sudden urge to urinate.
- Aging: As individuals age, changes in bladder capacity and muscle function can increase the likelihood of experiencing OAB symptoms. Age-related changes can affect bladder control and increase the frequency of urination.
- Bladder Irritants: Certain foods, drinks, and medications can irritate the bladder, exacerbating OAB symptoms. Common irritants include caffeine, alcohol, spicy foods, artificial sweeteners, and medications that increase urine production.
- Urinary Tract Infections (UTIs): Infections in the urinary tract, particularly recurring or chronic UTIs, can lead to irritation of the bladder and cause symptoms resembling OAB.
- Neurological Conditions: Diseases or conditions affecting the nervous system, such as Parkinson’s disease, multiple sclerosis, spinal cord injuries, or stroke, can disrupt the normal communication between the brain and the bladder, leading to OAB symptoms.
- Pelvic Floor Dysfunction: Weakness or dysfunction in the pelvic floor muscles, which support the bladder and control urination, can contribute to OAB symptoms, especially in women.
- Hormonal Changes: Fluctuations in hormone levels, particularly in women during menopause or hormonal imbalances, can affect bladder control and contribute to OAB symptoms.
- Psychological Factors: Emotional stress, anxiety, or psychological conditions can impact bladder function and exacerbate OAB symptoms.
- Obesity: Excess weight can put pressure on the bladder and pelvic organs, leading to irritation and increased urinary urgency and frequency.
- Chronic Constipation: Constipation can put pressure on the bladder and affect nerve signals, leading to symptoms similar to OAB.
Diagnostic Approach:
Diagnosing OAB involves a comprehensive assessment by a good urologist, which may include a detailed medical history, physical examination, urinalysis, and sometimes additional tests like urodynamic studies to evaluate bladder function. Accurate diagnosis forms the cornerstone for tailored treatment plans.
Investigations for OAB
Investigations for overactive bladder (OAB) aim to confirm the diagnosis, assess the severity of symptoms, and identify any underlying conditions contributing to the symptoms.
Physical Examination:
A physical examination helps rule out other potential causes of urinary symptoms and may include a neurological examination to assess nerve function that might impact bladder control.
Urinalysis:
A urinalysis helps detect urinary tract infections (UTIs) or other abnormalities in the urine that might contribute to symptoms similar to those of OAB.
Post-void Residual (PVR) Measurement:
PVR measurement assesses the amount of urine left in the bladder after voiding. It helps determine if incomplete bladder emptying is contributing to OAB symptoms.
Urodynamic Studies:
These specialized tests evaluate bladder function and can help diagnose OAB by assessing bladder capacity, pressure during filling, detrusor muscle activity, and bladder emptying. Urodynamic studies include:
Cystometry: Measures bladder pressure and capacity during filling.
Pressure Flow Study: Evaluates bladder pressure and flow rate during voiding.
Urethral Pressure Profile: Measures urethral pressure to assess urinary sphincter function.
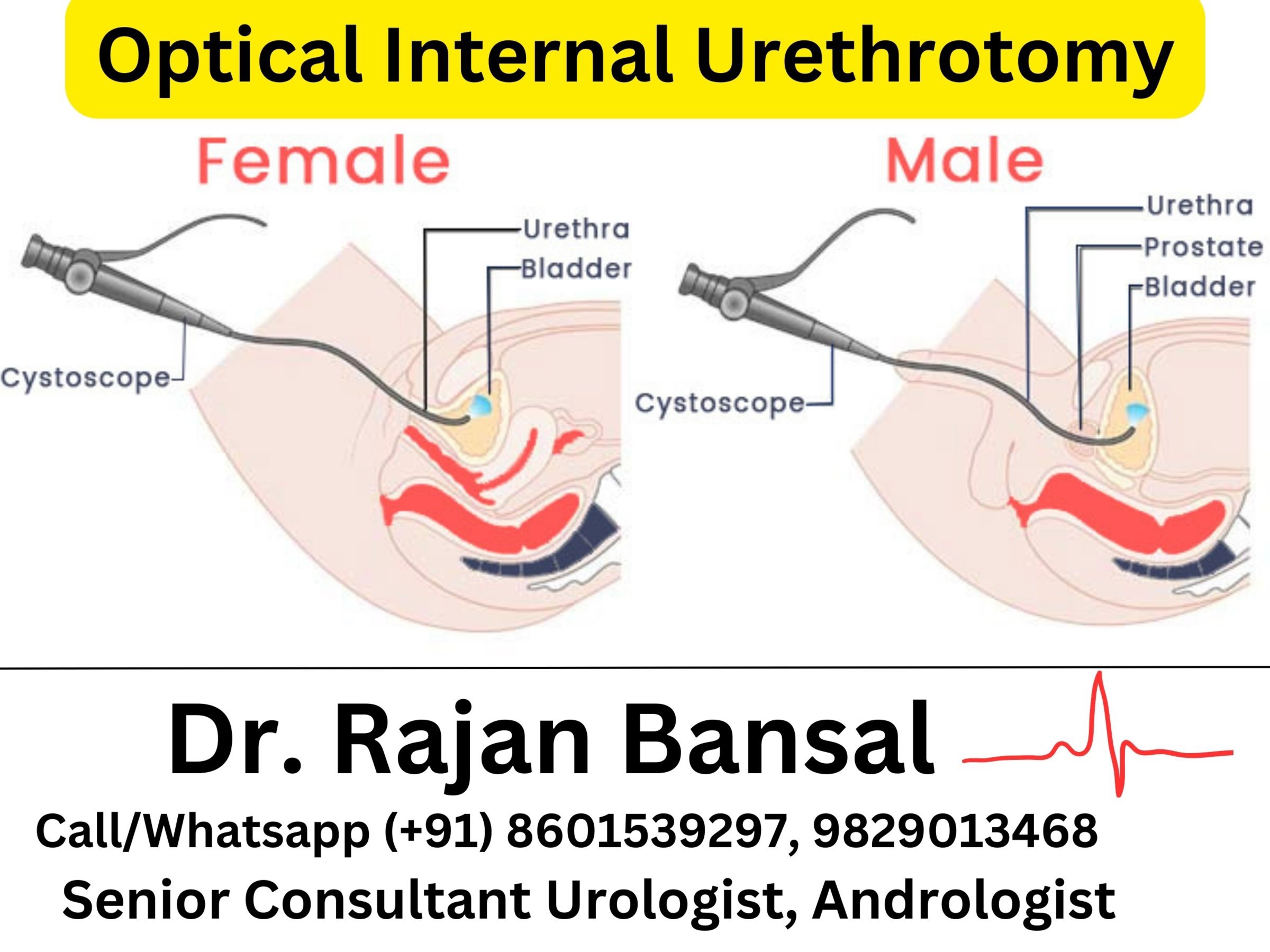
Cystoscopy:
Cystoscopy involves inserting a thin tube with a camera into the bladder to visualize the bladder wall and urethra. It’s not routinely performed for OAB diagnosis but may be done if other conditions are suspected.
Imaging Studies:
In specific cases, imaging tests like ultrasound, MRI, or CT scans may be ordered to evaluate the urinary tract for structural abnormalities or tumors that could contribute to OAB symptoms.
These investigations collectively aid healthcare professionals in confirming the diagnosis of overactive bladder, ruling out other potential causes, assessing the severity of symptoms, and tailoring treatment plans to address the specific needs of individuals experiencing OAB.
Treatment Modalities:
Managing OAB encompasses various treatment modalities tailored to an individual’s specific symptoms and underlying causes. Lifestyle modifications, such as fluid management, dietary changes, and pelvic floor exercises, can significantly alleviate symptoms. Medications targeting bladder muscle activity, nerve signaling, or anticholinergics may also be prescribed. For more refractory cases, advanced therapies like neuromodulation or botulinum toxin injections may be considered.
The treatment of overactive bladder (OAB) involves various approaches aimed at reducing symptoms, improving bladder function, and enhancing quality of life. Here are the common treatment options:
Behavioral Therapies:
Bladder Training: This involves scheduled voiding to gradually increase the time between bathroom visits, helping to improve bladder control.
Scheduled Toilet Trips: Setting a fixed schedule for voiding, regardless of the urge, can train the bladder to hold urine for longer periods.
Fluid Management: Adjusting fluid intake, avoiding excessive caffeine or alcohol, and maintaining a balanced hydration level can help manage OAB symptoms.
Pelvic Floor Exercises (Kegels):
Strengthening pelvic floor muscles through exercises recommended by a healthcare provider can improve bladder control and reduce urgency.
Medications:
Anticholinergic Medications: Drugs like oxybutynin, tolterodine, solifenacin, or fesoterodine help relax bladder muscles and reduce urinary urgency and frequency.
Beta-3 Adrenergic Agonists: Mirabegron is a newer class of medication that works by relaxing the bladder muscle, increasing bladder capacity, and reducing episodes of urgency.
Intradetrusor Injections:
Botulinum toxin injections into the bladder muscle can relax the muscle, reducing urinary urgency and frequency. This is usually considered for individuals who don’t respond well to oral medications.
Neuromodulation:
Sacral Nerve Stimulation (Interstim Therapy): This involves implanting a device that sends mild electrical pulses to the nerves controlling the bladder, helping to reduce symptoms.
Percutaneous Tibial Nerve Stimulation (PTNS): Involves stimulating the nerves in the ankle to improve bladder function.
Botox Injections:
Botulinum toxin injected into the bladder can relax the muscles and reduce urinary urgency and frequency, especially in cases resistant to other treatments.
Surgery:
Surgical procedures like bladder augmentation or urinary diversion may be considered in severe cases when other treatments have not been effective. However, these options are usually considered as a last resort due to their invasive nature and potential complications.
Combination Therapies:
Often, a combination of behavioral therapies, medications, and other interventions may be used to maximize effectiveness in managing OAB symptoms.
It’s essential to consult an expert urologist to determine the most suitable treatment plan based on individual symptoms, severity, and underlying causes of OAB. Treatment strategies are often personalized to address the specific needs and preferences of each person experiencing overactive bladder symptoms.
Holistic Management and Lifestyle Modifications:
A holistic approach to managing OAB involves empowering individuals with education and support, emphasizing the importance of healthy lifestyle modifications. Simple yet effective measures like maintaining a healthy weight, avoiding bladder irritants (caffeine, alcohol), and adhering to a regular toileting schedule can significantly improve bladder function and overall quality of life.
Overactive Bladder Treatment Best Hospital – Institute of Urology, C Scheme, Jaipur, Rajasthan
Overactive bladder, with its distressing symptoms and potential impact on daily life, necessitates a proper understanding and tailored management approach. By combining lifestyle modifications, behavioral strategies, and appropriate medical interventions, individuals can regain control, alleviate symptoms, and improve their overall well-being. Empowering patients with knowledge and effective management strategies is fundamental in addressing the challenges posed by OAB and enhancing their quality of life.
At Institute of Urology, Jaipur our main focus is to first establish the correct diagnosis. Once we do that, we offer comprehensive management of Overactive Bladder. The aim is to provide quick and long lasting relief and making sure patient does not have to face such issues again. Our team of experts Dr. M. Roychowdhury and Dr. Rajan Bansal are extremely understanding of the patient’s concerns and with their expertise, they are able to provide personalised treatment plans as per the best standards in a medical facility.
Now, we have also started the facility of online consultation so that you can discuss about your problems in detail with our experts from the comfort of your home. Please remember to keep ready all the investigations that you’ve had done so far so that it is helpful for the specialist to guide you precisely about the next course of action. At Institute of Urology, we strictly abide by the International protocols so that we keep up with the latest and best of what the advancements in the medical field has to offer.
Our doctors can be reached Monday to Saturday during working hours.
Dr. M. Roychowdhury – 9929513468
Dr. Rajan Bansal – 8601539297